Understanding Sinusitis: Symptoms, Causes, and Treatments That Work
If you’ve ever had a cold that just wouldn’t quit — the congestion lingering for weeks, the pressure building behind your face, the headaches that won’t let up — there’s a good chance you’ve experienced sinusitis. It’s one of the most common health conditions out there, affecting roughly 30 million Americans every year.
But what exactly is sinusitis? How is it different from a regular cold? And most importantly, what actually works to treat it? Let’s break it all down in plain language.
What Is Sinusitis?
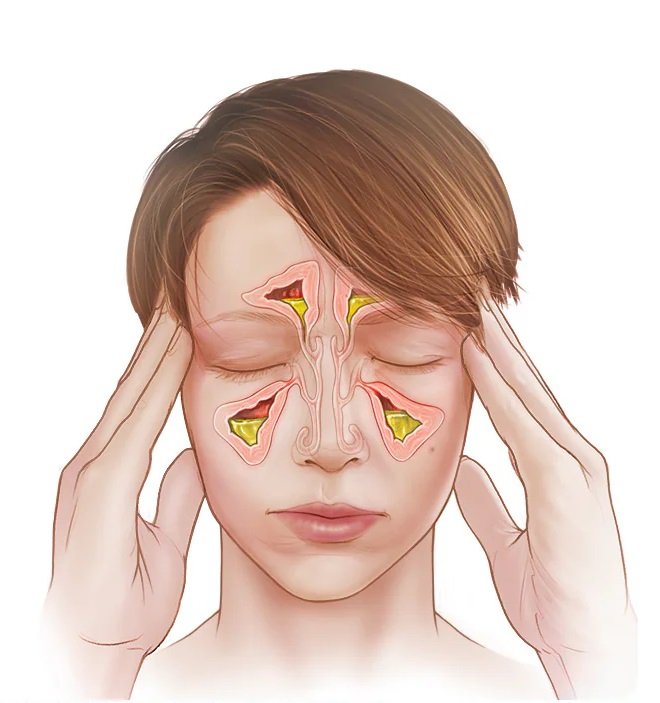
Sinusitis (also called rhinosinusitis) is the inflammation and swelling of the tissue lining your sinuses — the air-filled cavities behind your forehead, cheeks, nose, and eyes.
When these cavities are healthy, they’re filled with air. But when they become inflamed, the lining swells and blocks the normal drainage of mucus. That trapped mucus creates the perfect breeding ground for bacteria, viruses, and fungi — which is how a simple stuffy nose can turn into a full-blown sinus infection.
Acute vs. Chronic Sinusitis: What’s the Difference?
| Feature | Acute Sinusitis | Chronic Sinusitis |
|---|---|---|
| Duration | Less than 4 weeks | 12 weeks or longer |
| Most common cause | Viral infection (cold) | Persistent inflammation, polyps, or structural issues |
| Onset | Sudden, often after a cold | Gradual, lingering symptoms |
| Treatment | Usually resolves with home care | May require prescription medication or surgery |
| Recurrence | Occasional | Ongoing or frequently recurring |
There’s also subacute sinusitis (lasting 4–12 weeks) and recurrent sinusitis (4 or more acute episodes per year). Understanding which type you have helps determine the right treatment approach.
What Causes Sinusitis?
Several factors can trigger or contribute to sinusitis:
Infections
- Viral infections — the common cold is the most frequent cause. Cold viruses inflame sinus tissue, blocking drainage.
- Bacterial infections — develop as a secondary complication when trapped mucus gets infected. This is when antibiotics may help.
- Fungal infections — less common, but can cause chronic sinusitis, especially in people with weakened immune systems.
Allergies and Environmental Factors
- Allergies — pollen, dust mites, pet dander, and mold all trigger histamine release, causing sinus swelling
- Air pollution and smoke — irritate sinus tissue and increase susceptibility to infections
- Dry air — dehydrates nasal membranes, impairing normal mucus flow
Structural and Medical Factors
- Deviated septum — a crooked wall between your nostrils can block sinus drainage on one side
- Nasal polyps — soft growths that can physically obstruct sinus passages
- Weakened immune system — conditions like diabetes, HIV, or immunosuppressive medications increase infection risk
- Asthma — people with asthma are more prone to sinus inflammation
Sinusitis Symptoms: How to Tell It’s Not Just a Cold
A cold and sinusitis share some symptoms, but there are key differences that help you distinguish between them:
Primary Sinusitis Symptoms
- Facial pain and pressure — aching behind the cheeks, forehead, or between the eyes that worsens when bending forward
- Nasal congestion — that won’t budge no matter how much you blow your nose
- Thick, discolored nasal discharge — yellow or green mucus (a cold typically produces clear mucus)
- Reduced sense of smell and taste
- Post-nasal drip — mucus draining down the back of your throat
Additional Symptoms
- Sinus headache — deep, constant aching in your forehead or between your eyes
- Ear pressure or fullness
- Bad breath (halitosis) — from bacteria in trapped mucus
- Fatigue — your body is working hard to fight the infection
- Tooth pain — upper teeth can ache due to pressure from inflamed maxillary sinuses above them
- Cough — usually worse at night due to post-nasal drip
Key difference from a cold: A cold usually improves after 7–10 days. If your symptoms last beyond 10 days without improvement — or if they improve and then suddenly get worse — that’s a strong signal of sinusitis.
How Is Sinusitis Diagnosed?
Most acute sinusitis can be diagnosed based on your symptoms alone. But for persistent or recurring cases, your doctor may use:
- Physical examination — checking for tenderness around your sinuses and looking inside your nose
- Nasal endoscopy — a thin tube with a camera inserted into your nose to visualize the sinus openings
- CT scan — provides detailed images of your sinuses to identify blockages, polyps, or structural problems
- Allergy testing — if allergies are suspected as the underlying trigger
- Mucus culture — in rare cases, to identify the specific bacteria causing a chronic infection
Sinusitis Treatments: What Actually Works
The right treatment depends on the type and severity of your sinusitis. Here’s a comprehensive breakdown:
Home Remedies — The First Line of Defense
For most cases of acute sinusitis, home care is all you need:
- Saline nasal irrigation — the single most recommended home treatment. A neti pot or squeeze bottle flushes out mucus, allergens, and bacteria. See our review of the top 5 neti pot brands for help choosing one.
- Steam inhalation — breathe in warm, moist air for 10–15 minutes to thin mucus and reduce inflammation
- Warm compresses — place on your face to ease sinus pressure and pain
- Hydration — drink plenty of fluids to thin mucus (warm fluids like herbal tea for congestion are ideal)
- Rest — your immune system fights infections most effectively when you’re resting
- Head elevation — sleep with your head propped up to encourage sinus drainage
Over-the-Counter Medications
- Pain relievers (ibuprofen, acetaminophen) — reduce facial pain and headaches. Ibuprofen is preferred because it also fights inflammation.
- Decongestants (pseudoephedrine) — reduce nasal swelling. Avoid nasal decongestant sprays for more than 3 days (rebound congestion risk).
- Nasal corticosteroid sprays (fluticasone) — reduce inflammation. These are especially helpful for allergic sinusitis and can be used longer-term.
- Mucolytics (guaifenesin) — thin mucus so it drains more easily. Drink extra water when taking these.
Prescription Treatments
- Antibiotics — prescribed only for confirmed or strongly suspected bacterial sinusitis. Most sinusitis is viral, so antibiotics won’t help in most cases. If prescribed, always complete the full course.
- Prescription nasal corticosteroids — stronger anti-inflammatory sprays for moderate to severe cases
- Oral corticosteroids — short courses may be used for severe inflammation, especially with nasal polyps
- Allergy medications — if allergies are the underlying trigger, immunotherapy or prescription antihistamines may help
Surgical Options for Chronic Sinusitis
When chronic sinusitis doesn’t respond to medications or keeps coming back, surgery may be an option:
- Functional Endoscopic Sinus Surgery (FESS) — the most common procedure. A tiny camera and instruments are used to remove blockages and widen sinus drainage pathways.
- Balloon sinuplasty — a minimally invasive procedure where a small balloon is inflated inside the sinus passage to widen it
- Polyp removal — if nasal polyps are causing recurring blockages
- Septoplasty — corrects a deviated septum that’s contributing to drainage problems
How to Prevent Sinusitis
You can significantly reduce your risk of sinus infections with these daily habits:
- Practice regular nasal irrigation — daily saline rinses clear allergens and irritants before they cause inflammation
- Wash your hands frequently — most sinusitis starts with cold viruses spread through hand contact
- Manage allergies proactively — treat allergies before symptoms escalate into sinus inflammation
- Use a humidifier — maintain 30–50% indoor humidity to keep nasal passages moist
- Avoid cigarette smoke — smoking damages the cilia that help move mucus through your sinuses
- Stay hydrated — consistent water intake keeps nasal mucus thin and flowing
- Eat immune-boosting foods — vitamin C, zinc, and antioxidant-rich fruits and vegetables support your body’s defenses
- Don’t overuse decongestant sprays — limit to 3 days max to avoid rebound congestion
For more natural approaches to keeping your sinuses healthy, explore our guides on herbal remedies for nasal congestion and natural cures for sinus infections.
Potential Complications of Untreated Sinusitis
While most sinusitis resolves without complications, leaving severe or chronic cases untreated can lead to:
- Chronic sinusitis — acute infections that aren’t properly treated can become chronic
- Nasal polyps — chronic inflammation can promote polyp growth, creating a cycle of blockage
- Orbital cellulitis — infection spreading to the tissue around the eyes (a medical emergency)
- Meningitis — extremely rare, but infection can spread to the membranes covering the brain
- Reduced quality of life — chronic congestion, headaches, and fatigue affect work, sleep, and daily activities
These complications are rare but underscore the importance of treating persistent sinusitis symptoms rather than ignoring them.
Frequently Asked Questions
How do I know if I have sinusitis or just a cold?
A cold typically improves after 7–10 days. If your symptoms last beyond 10 days without getting better, involve thick yellow or green nasal discharge, or include significant facial pain and pressure, you likely have sinusitis rather than a simple cold.
Do I need antibiotics for sinusitis?
Usually not. About 70% of acute sinusitis cases are viral and resolve without antibiotics. Antibiotics are only effective against bacterial sinusitis. Current guidelines recommend waiting at least 10 days before considering antibiotics unless symptoms are severe (high fever, intense facial pain).
How long does sinusitis last?
Acute sinusitis typically resolves within 2–4 weeks. Subacute sinusitis lasts 4–12 weeks. Chronic sinusitis persists for 12 weeks or more and often requires more aggressive treatment. With proper home care, most people feel significant improvement within 7–10 days.
Can sinusitis go away on its own?
Yes, most cases of acute viral sinusitis resolve on their own within 7–10 days. Home remedies like saline rinses, steam inhalation, and rest can speed up recovery. However, if symptoms persist beyond 10 days or worsen, medical attention is recommended.
Is sinusitis contagious?
Sinusitis itself isn’t contagious, but the viruses and bacteria that cause it can be spread to others. If your sinusitis started with a cold, you can spread that cold virus through coughing, sneezing, or hand contact. Practice good hand hygiene and cover coughs and sneezes.